Toxic shock syndrome is a sudden and potentially fatal condition resulting from the toxins produced by bacterium Staphylococcus aureus and occasionally by group A streptococcus bacteria. This condition is most commonly found in women, typically affecting menstruating women who use super absorbent tampons. While the exact reason for this is not well known, it is thought that if super absorbent tampons are left in place for a long time, they can become a breeding ground for bacteria. Another possibility is that these tampons scratch the surface of the vagina, providing an opportunity for infection. The condition can also affect individuals using contraceptive sponges, menstrual sponges, cervical caps, and diaphragms. Women who have recently given birth are also at a higher risk for developing toxic shock. Individuals recovering from surgery, an open wound, or burn or those who use a prosthetic device are at a higher risk for exposure to Staphylococcus aureus, and may develop toxic shock syndrome. The incidences of non-menstrual cases of toxic shock syndrome are increasing, and it is important to remember this condition can affect children and men as well as women.
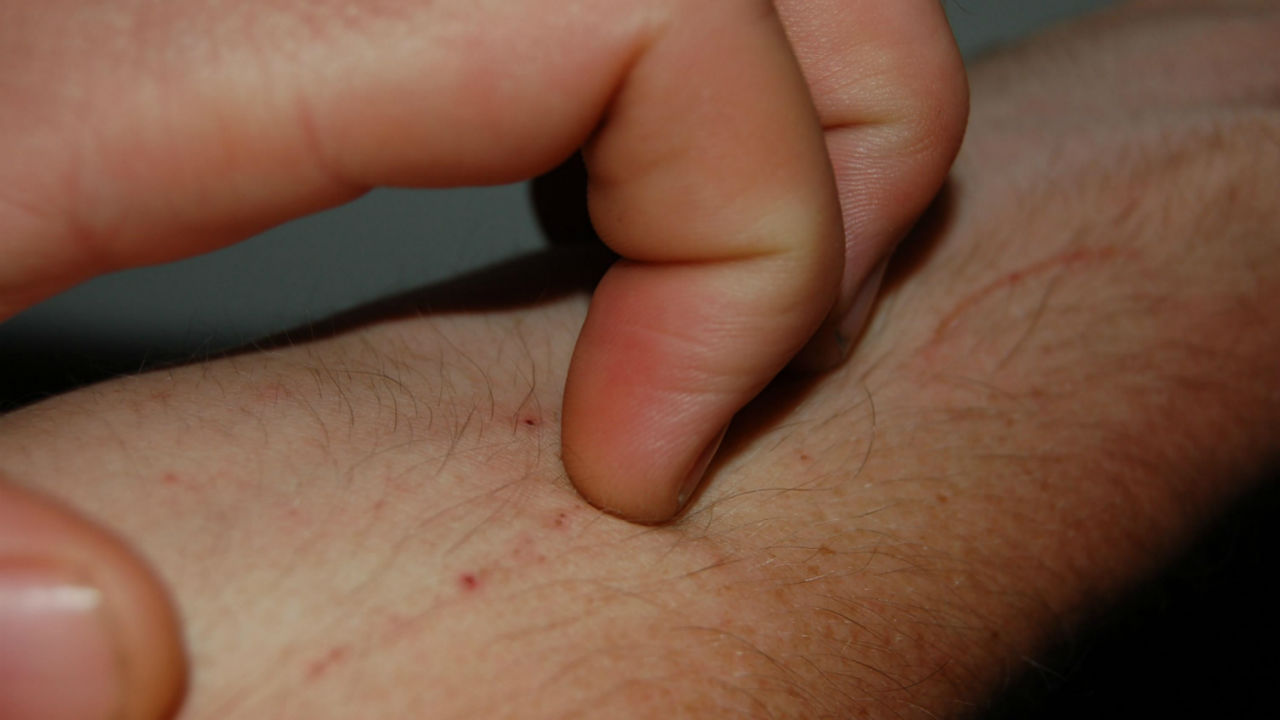
Patients suffering from toxic shock syndrome may have an initial two to three day period of minor symptoms before full development of the disease. Patients may experience the onset of a low grade fever, malaise, chills, and muscle aches. As the disease progresses, patients may experience an elevated fever (greater than 102°F) and the development of a rash. Toxic shock syndrome produces a red rash (similar to sunburn in appearance) that covers most of the body. The rash is flat and will turn white if pressure is applied. Development of this rash may be less pronounced on darker skinned individuals. Following development of a rash, individuals may experience redness of the tongue (strawberry tongue), lips, and eyes. Toxic shock syndrome can affect organs other than the skin, such as the lungs, liver, kidneys and pancreas, as well as affecting the blood. In addition to affecting the skin, toxic shock syndrome affects at least three other organ systems. Patients may experience vomiting, diarrhea, hypotension (low blood pressure), confusion, seizures, muscle aches, and headaches.
Treatment for toxic shock syndrome may require hospitalization, depending on the severity of infection. Treatment typically requires the use of antibiotics to treat the source of infection. Medication and supportive care may be used to treat the symptoms of toxic shock syndrome and prevent complications. Patients suffering from hypotension may require medication to stabilize blood pressure, and IV fluids may be used to treat dehydration. Dialysis may be required for patients who experience kidney failure as a complication of infection.
Toxic shock syndrome is a serious condition because the toxins produced from Staphylococcus aureus are lethal. Prevention is important for this condition because of its potential lethality. If you use tampons, try to change them frequently (between four to eight hours) and consider using lower absorbency tampons or alternative methods. If you are prescribed antibiotics following surgery or any medical procedure, it is paramount that you take them. If you have contracted toxic shock syndrome before, you can get it again. If you have experienced toxic shock syndrome, do not use tampons at all.
References:
1) http://www.emedicinehealth.com/toxic_shock_syndrome
2) http://www.mayoclinic.com/health/toxic-shock-syndrome/
Chris Gromisch is a Junior Chemistry major at Trinity College.




Add a Comment1 Comments
Thanks for this informative article. You did not discuss, however, the different types of tampons.
Philip Tierno Jr., chief of clinical microbiology and immunology at New York University Medical Center and a leading authority on tampon health risks notes in his recent book, The Secret Life of Germs, that over the past 30 years he has never seen a single case of TSS resulting from the use of a pure cotton tampon. He also states his belief that because viscose rayon offers up to 4 times more specific surface area than cotton, every case of TSS is caused in part by the use of this material.
Organic cotton tampons, like those made by Seventh Generation, contain 100% pure cotton grown without pesticides and not bleached with chlorine. Plus, they work just like conventional tampons.
You can get more information about organic feminine care at http://www.letstalkperiod.com.
July 22, 2010 - 8:15amThis Comment