Staphylococcal scalded skin syndrome is a severe skin condition caused by a staphylococcal infection. The infection is caused by the toxin exfoliatin (epidermolysin toxins A and B) produced by Group II coagulase-positive staphylococci (usually Staphylococcus aureus). These toxin bind to Desmoglein 1, part of the desomosome (the part of the skin responsible for adhesion to adjacent cells), causing the cells to become un-adhered. The condition is known as Ritter’s disease or Lyell’s disease when found in newborns or young infants.
Children younger than five years, and most commonly newborn babies, have the highest incidence of Staphylococcal scalded skin syndrome. During childhood, the body typically acquires immunity to staphylococcal exotins, reducing incidence in children and adults. Newborns typically lack specific immunity to toxins and coupled with immature renal clearance systems, newborns are at a higher risk for infection. Individuals who are immunocompromised or suffer from renal failure can develop Staphylococcal scalded skin syndrome at any age.
Infection of newborns and young children can result from infection by an adult carrier, making this a problem at childcare facilities. Approximately 15-40 percent of healthy humans are carriers to Staphylococcus aureus, carrying the bacteria on their skins without a sign of infection. Staphylococcus aureus has a higher infection rate amongst children, who typically do not have a strong immune system. These infections are most common in the eyes, ears, and throat and can increase the risk of Staphylococcal scalded skin syndrome.
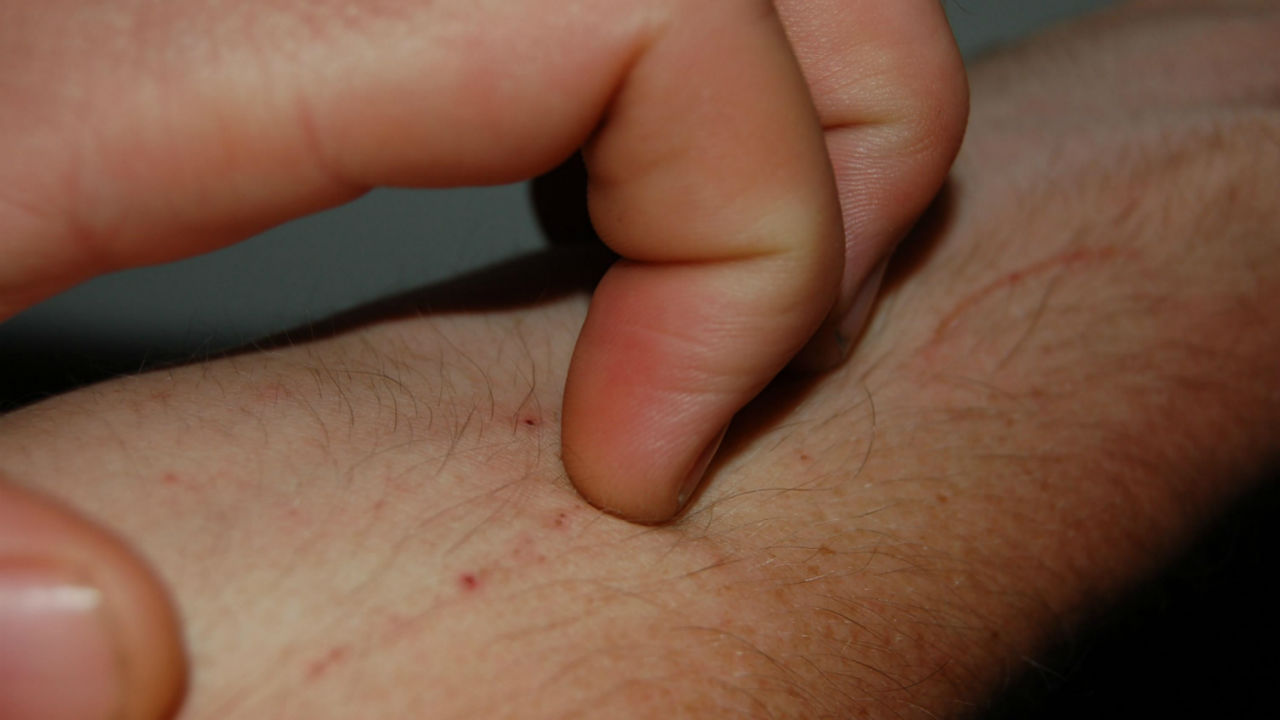
The onset of Staphylococcal scalded skin syndrome begins with lesions on the skin. Within 24 hours, these lesions spread, causing the skin to become scarlet and painful. The skin can appear wrinkled and fragile, becoming tender and brittle. This rash may spread to the arms, legs, and torso and in newborns can be found in the diaper region and around the umbilical cord. The formation of fluid filled blisters (bullae) can develop between 24 and 48 hours after the initial legion. These bullae can be found in the armpits, nose, ears, and groin. These blisters may rupture (either on their own or through agitation), producing erosions. These blisters will extend laterally with gentle pressure. Following blistering, the skin can begin to peel, sometimes in large sheets. Within 36 to 72 hours after the initial lesion, shedding of the outer skin layer begins to affect most of the body and individuals may experience chills, fever, and malaise. Desquamated areas can resemble burn wounds. Damage to or loss of skin can result in infection, sepsis, and fluid and electrolyte imbalance.
Staphylococcal scalded skin syndrome can be diagnosed by taking a skin biopsy or cultures (taken from the conjuctiva, throat, nasopharynx, and nose)for adults. Regular check-ups following birth and during childhood years can allow for early detection of Staphylococcal scalded skin syndrome. Treatment of Staphylococcal scalded skin syndrome requires the use of antibiotics and gel dressings for open lesions. Corticosteroids are generally not recommended for the treatment of young children. Depending on the severity of the condition, the skin may be treated similarly to burn treatments. If detected and treated early, patients generally do not die, and typically heal within five to seven days following the start of treatment. Staphylococcal scalded skin syndrome is a serious skin condition and it is important to take pre-emptive measures. Schedule check-ups for infants and small children to help with early detection. For individuals who are immunocompromised or suffer from renal failure, timely medical appointments are a must. Proper hygiene for infants and young children is important. If you notice you or your child experiencing any of these conditions, contact a physician immediately.
References:
1) http://dermnetnz.org/bacterial/scalded-skin-syndrome.html
2) https://www.merck.com/mmpe/sec10/ch119/ch119m.html
Chris Gromisch is a Junior Chemistry major at Trinity College




Add a CommentComments
There are no comments yet. Be the first one and get the conversation started!