Most skin rashes are nothing more than a nuisance, causing irritation or producing an unsightly blemish. However, certain skin rashes can be life-threatening. One such disorder is pemphigus vulgaris, an autoimmune disorder causing blistering of the mucous membrane and the skin. Patients with this condition produce IgG autoantibodies to a transmembrane glycoprotein (desmoglein 3), a protein responsible for adhesion in the skin cells. These antibodies produce an allosteric change in desmoglein 3, increasing the active plasmin in the area and decreasing cell adhesion, resulting in acantholysis and cell degradation. Pemphigus vulgaris can affect patients using certain medications, such as ACE inhibitors and chelating agents such as penicillamine, although this is a rare reaction. Pemphigus vulgaris can be found in all races at all ages, but is more common in middle age and older individuals and those of Middle Eastern or Jewish descent.
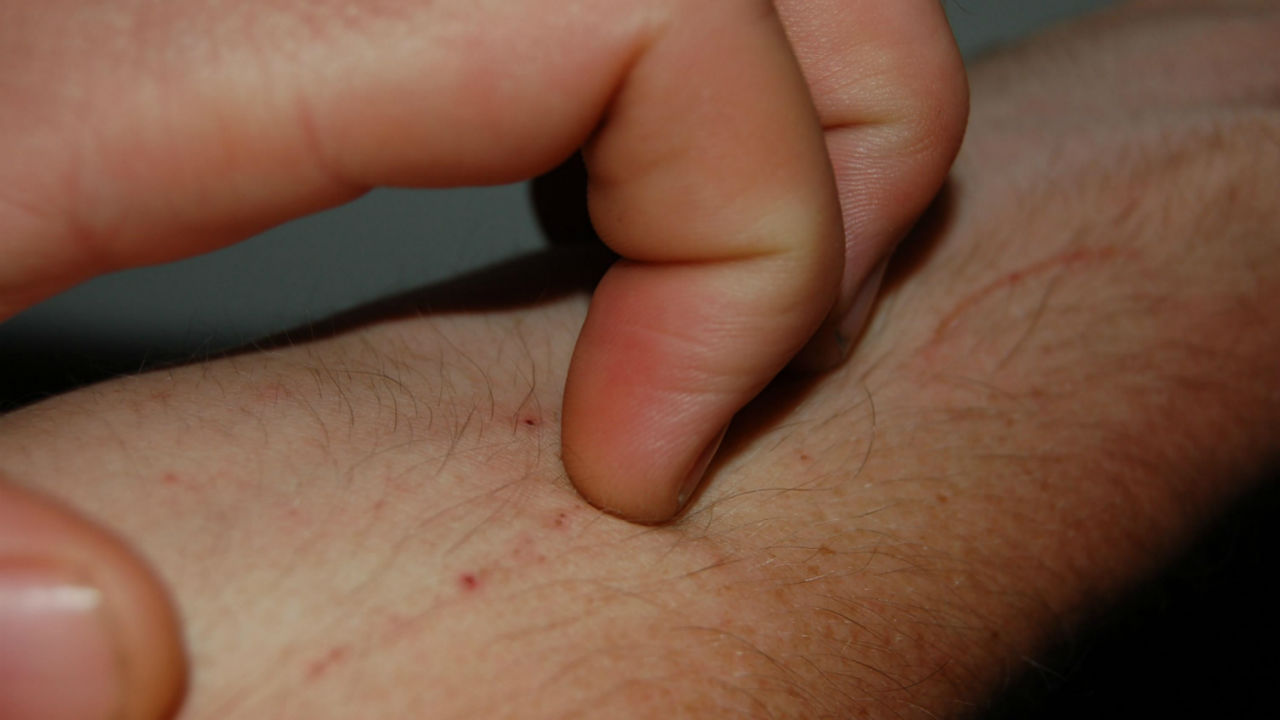
Pemphigus vulgaris is the most common form of pemphigus. Patients typically experience blisters in the mouth, which can spread onto the skin. Blisters can also appear on the mucous membranes of genitals as well as on the lining of the throat. These blisters can rupture easily, producing open sores that can ooze and become infected (a symptom characteristic to pemphigus). Rupturing of these blisters is exacerbated by scratching, which should be avoided if possible.
Two other forms of pemphigus include pemphigus foliaceus and paraneoplatic pemphigus. The former doesn’t affect the mucous membrane, and typically appears as crusted legions on the face and scalp, spreading to the chest and back. These legions are typically not painful, but can still rupture. Paraneoplastic pemphigus produces sores on the mouth and lip, within the esophagus in addition to skin legions. In some causes lesions can develop in the lung, causing progressive lung disease and dyspnea. This form of pemphigus is associated with certain forms of cancer.
Treatment of pemphigus depends on the severity of the individual case. Treatment of the condition mirrors treatment of severe burns, with some patients receiving treatment in the burn unit or intensive care unit. These patients may receive IV feedings (similar to ulcer treatment), as well as fluids, electrolytes, and proteins given intravenously. Anesthetic mouth lozenges may be given to reduce pain, and antibiotics and antifungal medication may be used to treat infection. Treatment of blisters may require certain topical medications or lotions as well as wet dressings. Systemic treatment is the most effective method, requiring the use of corticosteroids, dapsone, and certain immunosuppressants, such as azathioprine, methotrexate, cyclophosphamide, cyclosporine, or mycophenolate mofetil. Certain antibiotics have been found to be effective, such as doxycycline and minocycline, while the use of IVIg has also shown promising results. Plamsapheresis (a process that removes antibody-containing plasma and replaces it with donated plasma or IV fluids) can be used in addition with other medications to reduce autoimmune response.
Pemphigus is a serious condition, with generalized infection from the open sores being the most frequent cause of death. Even with treatment, the condition tends to be chronic and often disabling. Certain complications can arise from secondary skin infections (resulting from open sores), sepsis (the spread of infection through the blood stream), severe dehydration, and possible side effects from medication. Therefore, it is imperative to receive treatment as soon as symptoms develop. If any of the following conditions develop post treatment: fever, chills, muscle aches, joint aches, new blisters or ulcers, or a general ill feeling, contact a physician immediately.
References:
1) http://www.maxillofacialcenter.com/BondBook/mucosa/pv.html
2) http://www.mayoclinic.com/health/pemphigus/DS00749/DSECTION=causes
3) http://www.nlm.nih.gov/medlineplus/ency/article/000882.htm
Chris Gromisch is a Junior Chemistry major at Trinity College.




Add a Comment2 Comments
Pemphigus refers to a group of skin disorders that result in rankles on the skin. Natural Herbal Treatment support can take a variety of structures and blends. You may try of these Pemphigus Herbal Treatment that use only natural ingredients and simple instructions. Herbs Solutions By Nature offering Gesteton, an herbal products made out of natural ingredients that are got from genuine herb retailers.
http://www.herbs-solutions-by-nature.com/Pemphigus.php
August 17, 2016 - 2:04amThis Comment
I liked the article its very interesting and informative. Keep up the great work.
July 25, 2011 - 4:17amThis Comment